Orthopedic Care
From Total Joint Replacements to pediatric sports injuries, Tallahassee Memorial’s orthopedic surgeons are here to help you restore your quality of life with North Florida’s most comprehensive orthopedic care.
Orthopedic care focuses on treating injury or disease involving your musculoskeletal system – a network of bones, joints, muscles, ligaments, tendons and nerves. Tallahassee Memorial Orthopedic Center’s more than 20 skilled surgeons and their teams will provide you with the region’s most comprehensive orthopedic treatment, from pre-operative testing and surgery to post-operative care and recovery.

Having Joint Replacement Surgery at TMH?
Check out our total joint replacement education video to ensure you’re prepared for your surgery and post-operative recovery.
Watch Now
Pediatric Orthopedics
Learn more about the region’s first and most comprehensive orthopedic program for kids.
Learn MoreOrthopedic Services
Total ankle replacement surgery – also known as ankle arthroplasty – is a procedure to remove portions of the ankle joint and replace it with artificial parts.
Total hip replacement surgery — also known as total hip arthroplasty — is a procedure to remove severely damaged or diseased parts of your hip joint.
Total knee replacement surgery — also known as total knee arthroplasty — is a procedure to remove severely damaged or diseased parts of your knee joint and replace it with artificial parts.
Total shoulder replacement surgery — also known as total shoulder arthroplasty — is a procedure to remove severely damaged or diseased parts of your shoulder joint and replace it with artificial parts.
Managing and preventing osteoporosis and fragility fractures is one of the community’s greatest unmet health needs. That is why we have collaborated with physicians, surgeons and orthopedic staff to create the Own the Bone program.
Your children’s constant bone growth creates challenges as unique as they are. Tallahassee Memorial HealthCare is home to the region’s first and most comprehensive orthopedic program just for kids.
We offer innovative procedures, such as Lumbar Total Disc Replacement and Cervical Disc Replacement to help you maintain your mobility.
Our focus is to provide you with the highest quality treatment to help you get back to the playing field.
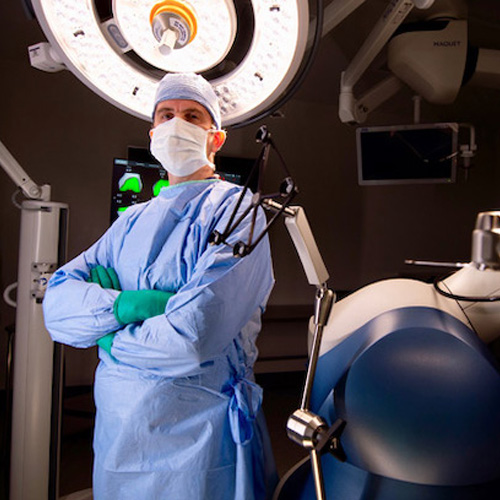
Bringing innovative technology to our region
Our use of Stryker’s Mako Robotic-Arm for knee replacement procedures is a leading approach to joint replacement that offers the potential for a higher level of patient-specific implant alignment and positioning. This means better outcomes for your knee replacement surgery.
Learn About the Mako Robotic-Arm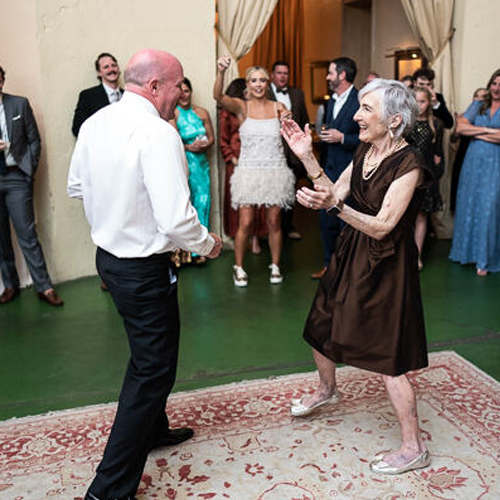
Transforming Your Quality of Life
When your joints and bones begin to ache, your quality of life begins to suffer. See how total joint replacement surgery made a transformative difference for one local patient and how she was back to being her old self in no time.
Read Lucile's Story
Nationally Recognized Orthopedics Care
Tallahassee Memorial HealthCare provides the highest quality orthopedics care in the region, and we have the accreditations to prove it. See what access to nationally recognized orthopedic care means for the health and safety our community.
Learn About Our Accreditations



